On The Front Lines
{{1-wide}}
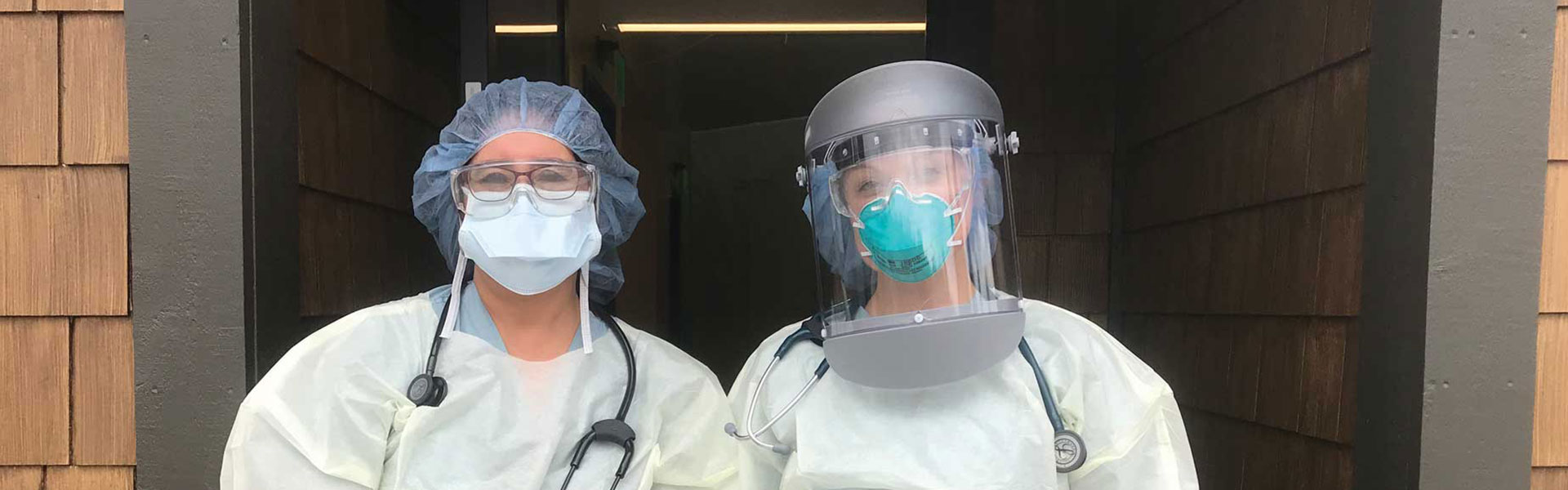
When nurse practitioner Carolyn Korfiatis ’05 arrived at work at her small rural hospital in Mammoth Lakes, California, she went through “the car wash.”
Created out of polyethylene plastic sheeting, the military-style decontamination chambers took Korfiatis and her colleagues through a series of rooms where they removed their street clothes, decontaminated and suited up for their shift.
{{2-right}}
Then at the end of the day, it reversed—hospital-issued scrubs came off, hand-washing and sterilizing began, and street clothes went back on.
In San Diego, California, emergency room resident Dr. Jessica Brice ’11 starts and ends her days in the emergency room in a similar fashion: an N95 mask and goggles, gloves and gown separate her from her patients. She covers her hair with a scrub cap. Her hospital clothes never leave the facility, and she removes her street clothes completely before entering the home she shares with her fiancé—heading straight to the shower before touching anything.
That’s what Dr. Mike Minkler ’09 does too. Minkler is the medical director of emergency services at Providence St. Mary Medical Center in Walla Walla, Washington. He has dedicated shoes that he only wears to work, as well as a dedicated shower area when he gets home.
Jamie Kuttler ’06, a physician assistant in Salt Lake City, Utah, wears a power air purifying respirator or PAPR. The large hoods that recirculate and filter the air look like something out of a post-apocalyptic movie.
The New Normal
In the spring of 2020, elaborate equipment, extra sterilization, and multiple layers of masks and gloves became the new normal for hospitals and health care workers around the globe as the novel coronavirus, commonly known as COVID-19, spread and surged.
For Whitman alumni working in health care, each day brought new challenges.
Dr. Barbara Cockrill ’81 isn’t just seeing patients in the intensive care unit (ICU) at Brigham and Women’s Hospital in Boston, Massachusetts, she’s also training future doctors as a Harold Amos Associate Professor and Director of Faculty Development for the M.D. Program at Harvard Medical School. When COVID-19 shut down in-person learning at Harvard in March, Cockrill and her colleagues transferred their 165-student homeostasis course online. When the course concluded in mid-April, she began a 12-day run of 12-hour shifts in the ICU, working with COVID patients.
{{3-left}}
“It was an enriching experience, to be so focused working closely with so many really dedicated people,” Cockrill said. “I’ve got to hand it to the nurses—they deserve all the credit. They’re the ones in the room, taking care of patients.”
Cockrill is a pulmonary vascular disease specialist, focusing on illnesses that impact the heart, blood and lungs. COVID-19 displays “classic pulmonary pathophysiology,” she said. One startling thing about the illness is the speed at which it strikes.
“It was surprising how quickly people got sick,” she said. “Patients would come in, they’d be doing OK, and then four to five days in, people would crash. They’d have to move them into ICU. They also stayed ‘sick’—on a ventilator—for a long time, longer than is typical for patients who develop this type of adult respiratory distress syndrome.”
Dr. David Mai ’11 said it felt like chaos when the outbreak hit the hospital in Chester, Pennsylvania, where he was finishing his emergency medicine residency last spring.
“It was difficult because it’s a new disease that really no one knew anything about,” Mai said.
Changing Our Health Care
As devastating and demanding as the pandemic has been, health care workers have noticed positives, too—such as an increased comfort with telehealth.
Korfiatis—who left Mammoth Lakes for a position at the Walla Walla Clinic in August—saw telehealth immediately benefit her patients in the rural California community, which is a 20-minute drive from the entrance to Yosemite National Park and famous for its ski resort, which often plays host to the U.S. Olympic ski team.
{{4-right}}
“We rolled out telemedicine visits, and I did 16-20 visits like that a day with my patients,” Korfiatis said. “You can’t touch patients, or hear their lungs or look at their skin rash, which is obviously limiting. But several of our patients drove really long distances, so I saw that it was really beneficial for them, as well as for those who needed general screening visits.”
Accessing health care through a video call is also easier for those patients with anxiety issues, she said, and as a way to do an early visit with a specialist that might be located further way.
“I actually do see it as being the wave of the future for primary care,” Korfiatis said.
In Walla Walla, Minkler said Providence Health & Services, which runs the local hospital, is bolstering its virtual platforms and will continue to invest and promote telemedicine. Even before the pandemic, Walla Walla neurologists used telemedicine to see patients who lived out of the area.
We Can't Thank Them Enough
Something else that hasn’t gone unnoticed: The outpouring of support that health care workers have seen around the nation.
“It’s been mind-blowing in San Diego. I literally did not bring food to work for weeks and weeks,” said Brice. Every day, restaurants would drop off meals for those working in the hospital. Community members decorated the entrance to the facility, and local first responders even came out with a “thank you” message. “The community has really rallied together.”
{{5-right}}
In Mammoth Lakes, each night at 8 p.m. the community gave a “howl for health care workers,” in which people around the small mountain town stood on their porches to give a wolf-like howl into the moonlight.
“My kids really looked forward to it,” Korfiatis said. “My patients were all amazing there. They, without fail, asked me how my family was and how I was doing. We had a lot of amazing support.”
As shortages of personal protective equipment (PPE) made national news, community members stepped up to help there too. For example, Kuttler said church groups in Salt Lake City created masks and gowns for health care workers.
And in Walla Walla, community organizations, government agencies and private donors—including Whitman Senior Lecturer of Chemistry Deberah Simon—came together to fund the purchase of a COVID-19 rapid testing machine.
We're in This Together
{{6-left}}
Health care providers are hopeful that continued distancing behaviors, mask-wearing, increased ability to test patients and an eventual vaccine will all help in combating COVID-19. But many unknowns remain.
“Until we have a vaccine, we’re going to have to be living with masks and social distancing,” Cockrill said. She worries not only about her patients, but also about her students at Harvard. She’s also concerned about the winter flu season, and how that will complicate the medical landscape.
She wants to see mask-wearing and social distancing lose its political edge.
“I just hope that people take the social distancing and wearing masks and respecting each other well enough so that we can stop another surge,” Cockrill said.
Health care workers recognize that asking for continued isolation is hard, but they ask the public to remember the health of the greater community.
“I think it’s really important, to the best of people’s abilities, to limit the social interaction that they have with one another, especially in big groups,” Mai said. “You may be healthy enough to combat this virus if you were to get it. However, you might end up spreading it to one of your loved ones who may be immunocompromised and therefore may be unable to fight this virus on their own.”